Multilayer Compression Improves Skin Quality in CVI: 10-Patient Series
Case series examining how modern multilayer compression wraps with pressure indicators improve skin quality and comfort in CVI patients.
Damon Ebanks
Medipyxis
Medical education note: This article is for clinicians and is not a substitute for patient-specific medical advice.
Why Chronic Venous Insufficiency Is So Tough on Skin
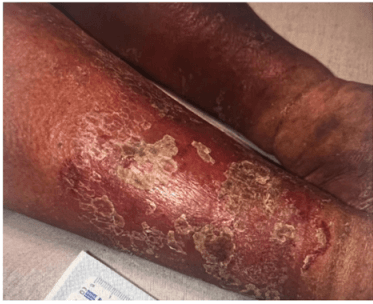
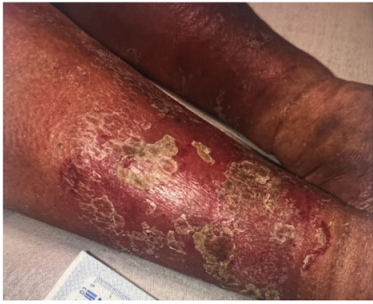 59-year-old male with history of arterial fibrillation, venous insufficiency, COPD and type 2 diabetes.
59-year-old male with history of arterial fibrillation, venous insufficiency, COPD and type 2 diabetes.
When leg veins fail to return blood effectively, pressure accumulates in the lower legs. Over time, chronic venous insufficiency (CVI) causes visible skin changes including hemosiderin staining, atrophie blanche, lipodermatosclerosis, venous eczema, and thickened, itchy skin around the ankle and gaiter area.
These inflammatory and fibrotic changes reduce skin elasticity and increase fragility. Patients often describe tight, woody legs that hurt and itch; once the skin barrier breaks, they face high risk of developing venous leg ulcers that heal slowly and recur frequently.
Compression Therapy: The Foundation of CVI and Venous Ulcer Care
Research spanning decades demonstrates that compression therapy serves as the primary treatment for venous leg ulcers and a cornerstone for preventing new ulcers in CVI patients. Appropriate compression (stockings or bandages) can heal 50–75% of venous ulcers when combined with good wound care and risk-factor management.
Multilayer and multi-component compression systems generally outperform single-layer wraps at reducing edema and improving healing rates by delivering more sustained, graded pressure and better calf-muscle pump support.
What Makes a Multilayer Compression System "Next-Generation"?
Modern two-layer and multilayer compression wraps often combine a soft or knitted base layer with a cohesive outer bandage. Many newer systems incorporate printed pressure indicators allowing staff to pull to standard tension and achieve more consistent sub-bandage pressure from visit to visit while reducing bandage slippage.
Clinical studies of these newer two-layer systems report rapid venous leg ulcer healing, reduced edema, improved health-related quality of life, and good tolerability compared with traditional four-layer or single-layer bandages.
Inside the CS-044 Case Series: 10 Patients, One Multilayer System
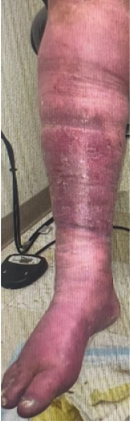 Same patient on day 14 after application of multilayer compression dressing.
Same patient on day 14 after application of multilayer compression dressing.
This case study presents ten patients with long-standing venous insufficiency and significant skin changes who transitioned to a novel multilayer venous compression wrap designed with a knitted base layer and pressure indicators.
These patients had all received previous compression treatments but continued displaying classic CVI skin findings such as atrophie blanche, lichenified plaques, hemosiderin staining, lipodermatosclerosis, and venous eczema before trying the new system.
After switching, every patient reported that the new multilayer dressing stayed in place, felt comfortable to wear, and improved perceived skin quality on the lower leg—suggesting better adherence and less day-to-day frustration with slipping bandages.
From a clinical standpoint, the multilayer compression system improved skin quality and may help prevent progression to chronic venous ulcers by supporting consistent, tolerable compression over time in people with advanced CVI changes.
Practical Tips for Using Multilayer Compression
Before applying a multilayer system, conduct a full lower-leg assessment: confirm wound or skin changes are primarily venous, measure ankle-brachial index or toe pressures to rule out severe arterial disease, review cardiac status, and document baseline edema and skin change patterns.
Have a straightforward conversation with patients about what compression will feel like, how long they'll likely need it, and what warning signs to watch for—such as sudden pain, numbness, or color change—which should trigger immediate review rather than waiting.
When using bandages with pressure indicators, follow manufacturer instructions to stretch until printed shapes line up correctly; this visual cue helps standardize sub-bandage pressure across different clinicians.
Track early patient response: within days to weeks, many notice less itching, reduced weeping, softer tissue, and fewer sock marks around ankles.
Limitations
CS-044 is a small, uncontrolled case series: ten patients, no comparator group, and no formal scoring of skin quality or quality of life, so findings should be viewed as hypothesis-generating.
Bottom Line
CVI slowly transforms lower-leg skin—causing staining, thickening, and lipodermatosclerosis that hurt, itch, and set the stage for venous leg ulcers. Modern multilayer compression systems with pressure indicators and low-slippage designs can make compression more consistent and comfortable, supporting better adherence and ultimately healthier skin.
References
- Multilayer compression case series CS-044. SAWC Fall 2025.
- O'Meara S, et al. Compression for venous leg ulcers. Cochrane Database Syst Rev.
- SVS/AVF Clinical Practice Guidelines: Management of venous leg ulcers. 2014.